How a House Finch Disease Reshaped What We Know About Epidemics
By Andrea Alfano December 2, 2013
Microbes may be tiny, but that doesn’t stop some of them from causing major destruction. Even supervillains like Lex Luthor or Doctor Doom were never able to pull off as much devastation as the bugs that cause bubonic plague or malaria. Comic book supervillains come with a backstory, but what is it that turns some microbes into monsters? Until recently, all scientists could do was make educated guesses.
It turns out it’s hard to find a good opportunity to study harmful, contagious diseases. It’s just not safe. One option is to study an epidemic that doesn’t affect humans—but then it’s hard to track the disease, since animals don’t check into hospitals. Fortunately, some scientists have an extensive network of dedicated citizen scientists to help them.
That’s how one team of researchers was able to study a highly virulent disease in House Finches. Their recent paper in PLOS Biology sheds light on what makes some disease-causing microbes, or pathogens, more harmful than others.
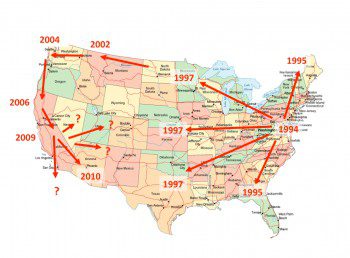
In February of 1994, Project FeederWatch participants in the Washington, D.C., area began reporting that House Finches at their feeders had swollen, red, crusty eyes. Lab tests revealed that the birds had Mycoplasma gallisepticum, a pathogenic bacterium that causes a form of conjunctivitis known as House Finch eye disease. The disease spread rapidly across the Eastern Seaboard, leaving House Finches listless, mostly blind, and vulnerable to predators and bad weather. (Where did the disease come from? See Jumping the Species Barrier.)
“At that time, there was a big panic that this disease would spread to migratory birds that would go to South America, and then all the birds there would get eye infections,” says André Dhondt, who is director of Bird Population Studies at the Cornell Lab and an author of the study.
Dhondt and his colleagues realized that if they were to have any chance of preventing such a disaster, they needed to learn more about this microbial menace. So they called upon their network of FeederWatchers and created a new citizen-science project called the House Finch Disease Survey entirely devoted to tracking the disease. (The survey has now merged with FeederWatch—participants are urged to take a second look for symptoms in any House Finches at their feeders.)
Using both citizen-science data and laboratory experiments that tested virulence levels, researchers found patterns they didn’t expect. They saw that the disease had become less virulent as the birds carried the disease westward and into areas with sparser finch populations. But after it became established on the West Coast, where human and House Finch populations are denser, the disease rapidly became more harmful again—just like it had in the East. The pattern was in direct conflict with a long-standing hypothesis that a pathogen would tend to decrease in virulence over time, in order to avoid killing its host before it could be transmitted.
But to understand what drives the evolution of virulence, you have to look at things from the perspective of the bacteria, says Dhondt. “If I’m a bacterium, what do I need to do in order to be successful? If I become too virulent and kill my host before I transmit, that’s not good. But if I don’t make my host sufficiently sick, I won’t be transmitted, and that’s not good either.” That’s the idea behind the newer “trade-off” hypothesis of virulence that was developed in the 1980s and 1990s, but has remained largely untested until now. In contrast to the earlier hypothesis, this one posits that virulence may increase or decrease over time in response to conditions that affect transmission.
In other words, it’s not that pathogens are truly evil or bent on destruction of their hosts. “Any harm that a pathogen does to its host is basically a byproduct of the need to transmit,” says Dana Hawley of Virginia Tech, the study’s lead author. Virulence and transmission are inextricably linked for pathogens because both increase as the pathogen makes more copies of itself within its host.

The pattern in virulence levels observed in House Finches make sense in light of the trade-off hypothesis. In regions where the finches were more sparsely distributed, any given finch is less likely to come into contact with another finch. A very sick, weak finch is even less likely to come across another finch, because it won’t be moving around as much.
But in order for the pathogen to get transmitted, the sick finch must come into contact with another potential host. As a result, in sparse populations only pathogens with lower virulence get transmitted. In evolutionary terms, sparse host populations select for lower virulence. The inverse of this is true as well, as shown by the fact that the bacteria became more virulent not only initially in the East, but once again in the denser populations of the West Coast.
House Finch eye disease ended up killing off half of all House Finches in eastern North America, a testament to the destructive power of epidemics. A true understanding of how pathogens like M. gallisepticum come to be such powerful forces is crucial to preventing future epidemics among humans. This new research is a major step toward achieving such an understanding, and citizen-science data was a key part of the solution. If citizen scientists can help us combat some of the world’s most powerful villains, one has to ask: What else are they capable of?
In addition to Hawley and Dhondt, the authors of this study include Erik Osnas and Andrew Dobson of Princeton, Wesley Hochachka of the Cornell Lab, and David Ley of North Carolina State University.
(This post was written by Cornell University senior Andrea Alfano. Images: map courtesy of Project FeederWatch; healthy finch on green background by Gary Tyson.)

All About Birds
is a free resource
Available for everyone,
funded by donors like you
American Kestrel by Blair Dudeck / Macaulay Library




